Enterprise Mobility & the Connected Worker Blog
For Better Care, Hospital at Home Programs Will Rely on Mobile Technology
Hospital at Home has presented a solution to capacity and patient experience challenges that have plagued the healthcare industry in recent years. Hospital at Home, a remote alternative to in-hospital care for recovering patients, can enable a more comfortable recovery environment for patients and a lower-cost, lower-resource option for healthcare providers. Hospital at Home models have been found to lead to faster patient recovery times and fewer relapses, saving patients and healthcare providers time and resources.
According to VDC’s Enterprise Buyer Behavior Guide, adapting to telehealth and remote health services was a top priority among healthcare industry technology leaders in 2022. Not only did the COVID-19 pandemic lay bare the weaknesses of hospital infrastructure, but it also overloaded hospitals and propelled healthcare leaders to evaluate alternative care models. Hospital at Home is a growing model among larger hospitals and enables patients to recover in their homes with the support of remote vitals monitoring, periodical video calls, and check-in visits.
What are the most significant obstacles facing the healthcare industry in general?
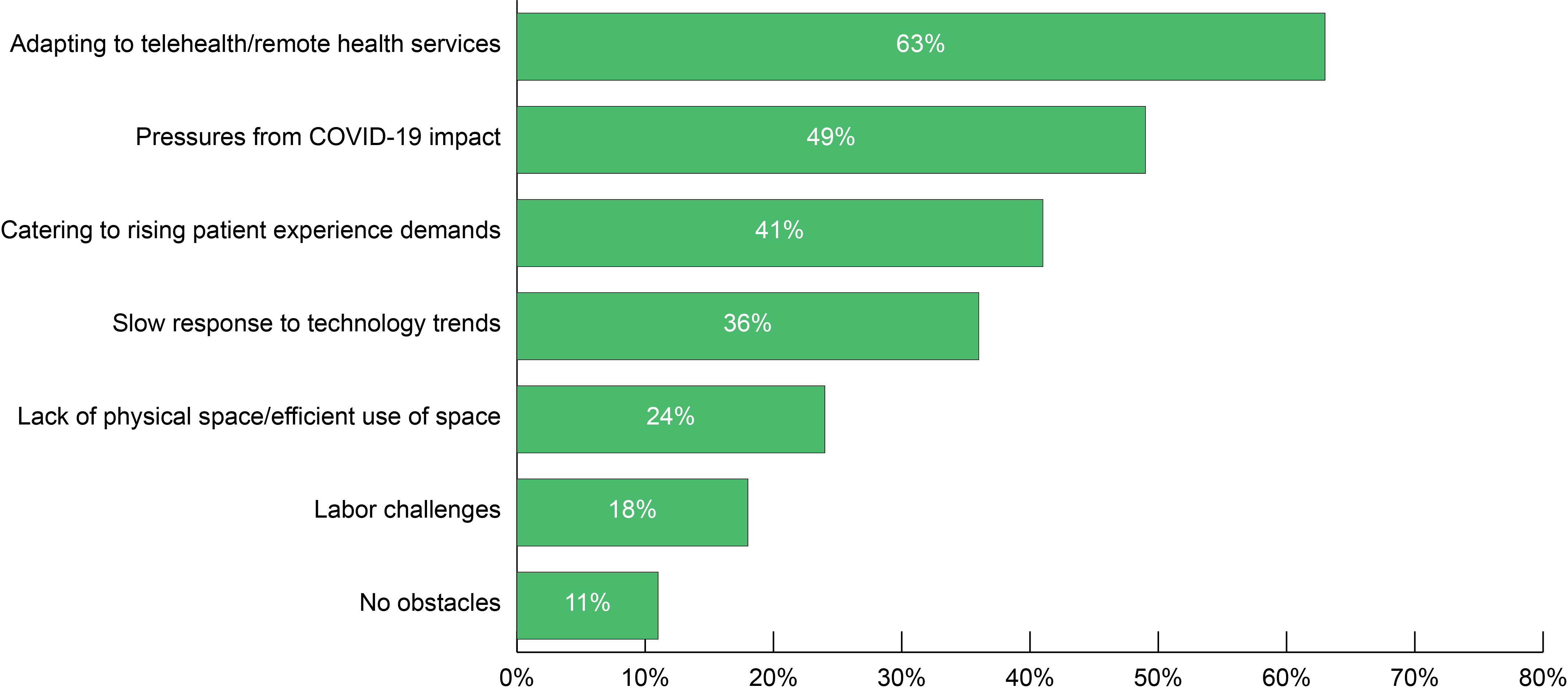
Enterprise Buyer Behavior Guide, 2022 (VDC Research)
The Hospital at Home model has the potential to change workflows inherent to the recovery process. Care providers’ schedules will be hybridized to incorporate patient visits, or certain roles will become dedicated to monitoring remotely recovering patients. The model, while lauded as cost-effective, also externalizes some labor expectations (and costs) to patients’ caregivers, who are mostly family members. Caregivers must learn to use and troubleshoot remote monitoring equipment, on top of addressing patients’ nonmedical recovery needs. Thus, the enterprise mobility model for Hospital at Home programs is dynamic and must prioritize technology ease of use above all other elements, due to the wide range of patients and family members who will be involved in equipment use.
For Hospital at Home programs to function, there must be an ecosystem of consumer devices, in-hospital rugged devices, and centralized data repositories. Patients, who may use remote monitoring wearable devices to track heart rate, blood pressure, and other vitals, can also message hospital workers via downloaded apps or via text. Mobile hospital staff can monitor patient vitals on mobile devices like rugged tablets and mobile computers. Data between patient apps and hospital staff’s devices is synchronized, enabling easy access to data and follow-up tasks. Finally, specialists needing to analyze patient progress and vitals can use laptops and mobile terminals to administer care.
While the program offers a cost-effective recovery solution for both patients and hospitals, Hospital at Home can be challenging to scale depending on a hospital’s size and a patient’s resources. For example, smaller hospitals may not have the staff or programmatic resources to launch a Hospital at Home program. The program, though cost-effective, is only possible for patients with certain resources: remote care is only possible with reliable internet connectivity in a patient’s home, and there must be relatives or other caregivers in the patient’s network willing to provide elements of in-person care. Some hospitals also face challenges around the safety of patients’ homes and potential liabilities involved in deploying medical staff to them.
VDC View
Remote monitoring technology will remain a crucial element of the Hospital at Home care model. OEMs serving the industry must be mindful of how Hospital at Home will shift workflows as hospitals will dedicate certain personnel to handling remote patients. Some new positions, such as patient technology and wearable monitoring, may be fully remote, enabling vulnerable workers (such as those who are older, pregnant, disabled, or otherwise immunocompromised) to take on responsibility within dedicated Hospital at Home programs. Other positions will require more travel to patients’ homes – for nurse and assistant roles, hospitals may opt to fully dedicate workers or subcontract to in-home care companies for a Hospital at Home program, rather than split their work between hospital and home environments. OEMs like Zebra and HP have already begun to prioritize serving Hospital at Home programs, prioritizing device ruggedness and data integration to ensure the success of the Hospital at Home model.
VDC’s 2022 Enterprise Buyer Behavior Guide discusses the major trends and motivators around device purchasing across seven industries.
Stay tuned for VDC’s 2023 Enterprise Buyer Behavior Guide, which will be published in Q4 2023.